The Context
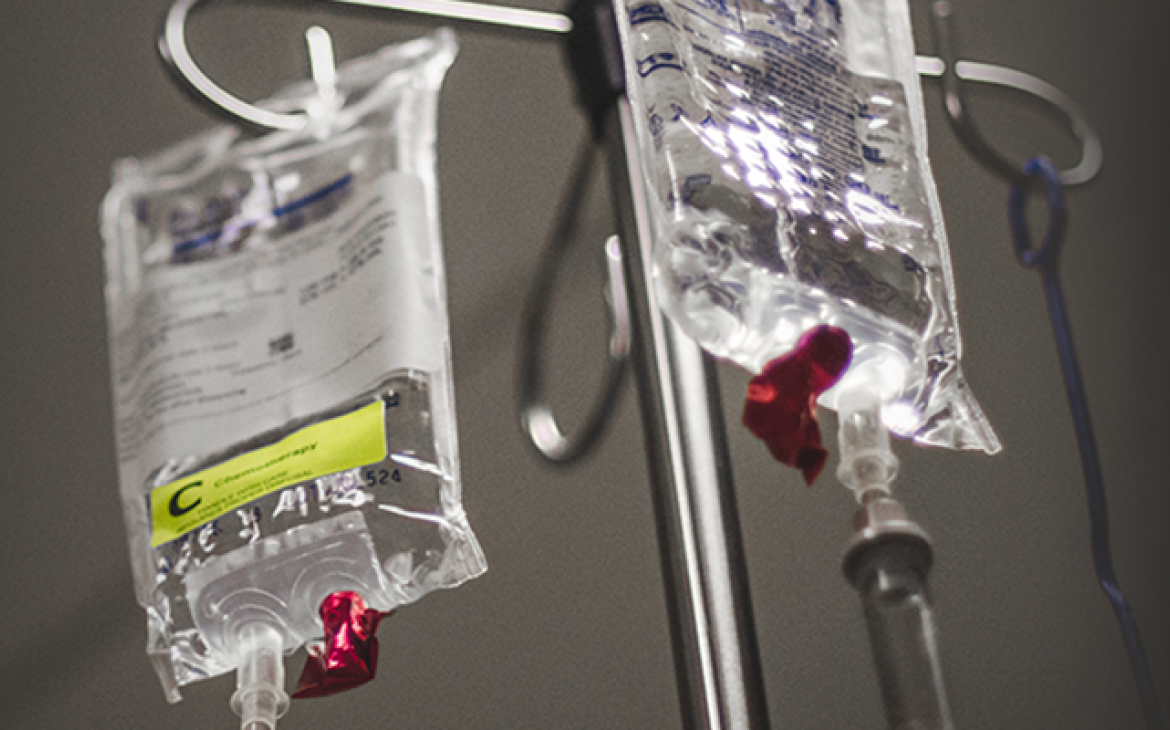
In the global race to procure vaccines, India—the world’s leading supplier of generic medicines—faces an acute shortage of COVID-19 vaccines. Often dubbed the world’s pharmacy, India must now obtain enough vaccines for its own people. The federal government is in charge of procuring COVID-19 vaccines. However, significant challenges in quality assurance—including storage, distribution, and getting shots into arms at the last mile—remain at the state level.
A country’s public health system must ensure its population has equitable access to safe, effective, affordable, quality-assured essential medicines and vaccines. As COVID-19 continues to spread in India, risking the emergence of new and more transmissible variants, incidents of substandard and falsified (SF) medicines are also on the rise. In June of this year, over 2000 people received falsified COVID-19 shots at a fake vaccination drive. SF medicines can prolong disease and suffering and result in severe illness and even death.
U.S. Pharmacopeia (USP) collaborated with Kerala Medical Services Corporation (KMSCL), a state government-owned medicines procurement organization, to identify best practices for strengthening quality assurance in state-level public procurement. Individual Indian state governments can now adopt these learnings in the context of COVID-19 vaccines and treatments.
Challenges
The public procurement system in India has been facing several challenges, including fragmented procedures, lack of transparency, irregularities, and unavailability of sufficient human resources.
Lack of access to quality-assured medicines increases out-of-pocket healthcare expenditures, about 70 percent of medical costs in urban and rural India, pushing about 38 million people below the poverty line. (1, 2) According to the national drug survey (2014-16), the prevalence of Not of Standard Quality (NSQ) was around 10.02% in the public system. Public procurement has immense potential to improve progress towards universal health coverage, but only if medicines are quality-assured.
While federal procurement of COVID-19 vaccines and treatments ensures timelier access and more reliable distribution—states are often ill-equipped to assure the quality of medical products. Strengthening existing quality assurance systems will be necessary, requiring programmatic expertise for population estimation, preparedness for mass vaccination drives, securing the supply chain and transport channels, allocation of human resources, building capabilities of front-line public health workers, and monitoring capacity.
Learning from the Kerala report can help strengthen quality assurance for procurement of essential medicines and distribution of vaccines procured by the State from the federal government.
Solutions: Key Learnings
Mapped against these five steps of procurement, the Kerala model highlighted key learnings and findings along the way:
- Revision of the Essential Medicines List: Kerala revises the essential medicines list (ELM) regularly, either once or twice a year, by engaging a multistakeholder committee that includes representatives from KMSCL, the departments of health and education.
- Estimation of annual demand: Demand is estimated using a consumption-based approach based on past consumption of health facilities.
- Supplier selection and management: Kerala requires suppliers to follow WHO good manufacturing practice (GMP) and identifies which medicines must be kept in the cold chain. Also, KMSCL centralizes the tendering process through a single portal to make it efficient, transparent, and reliable.
- Quality control and management: KMSCL engages a network of private laboratories for quality control sampling and testing and verifying supplier certificates of analysis. Further, warehouses supply medicines downstream only after providing quality assurance.
- Storage, inventory management, and distribution: KMSCL emphasizes teamwork and continuous improvement to optimize medicines storage space and time spent in warehouses; temperature monitoring is in progress.
Some of the driving factors for KMSCL’s high performance included leadership, robust review mechanisms, coordination among various government departments, information technology systems, and operating within a developed social context. KMSCL can serve as an example for other states to enhance their public health capabilities.
Moving Forward
The Kerala report emphasizes the need for strong procurement policies, scientific storage, inventory management practices, and quality control by ensuring staff accountability. As states procure COVID-19 vaccines and other essential medicines, they can look to this report for lessons to adapt and apply to their context.
Based on the finding of the Kerala report, USP makes the following recommendations to apply best practices in the context of COVID-19.
- Pooled procurement systems should adhere to basic approaches to assure quality, such as supplier selection, quality control indicators, storage, inventory management, and distribution. Field-based screening technologies are also needed to ensure vaccine quality.
- Each state should have robust systems for estimating demand for COVID-19 treatments and essentials, particularly oxygen, when cases rise and peak. There is an urgent need to expand cold-chain equipment, storage, and transport facilities in the country.
A transparent public procurement system can prevent, detect, and respond to essential substandard and falsified medical products. Best practices in state-level procurement can help in efforts to assure medicines quality for all.
Read about this collaboration between USP and KMSCL by downloading the full report. For more information, please contact Dr. Kishor Mogulluru.