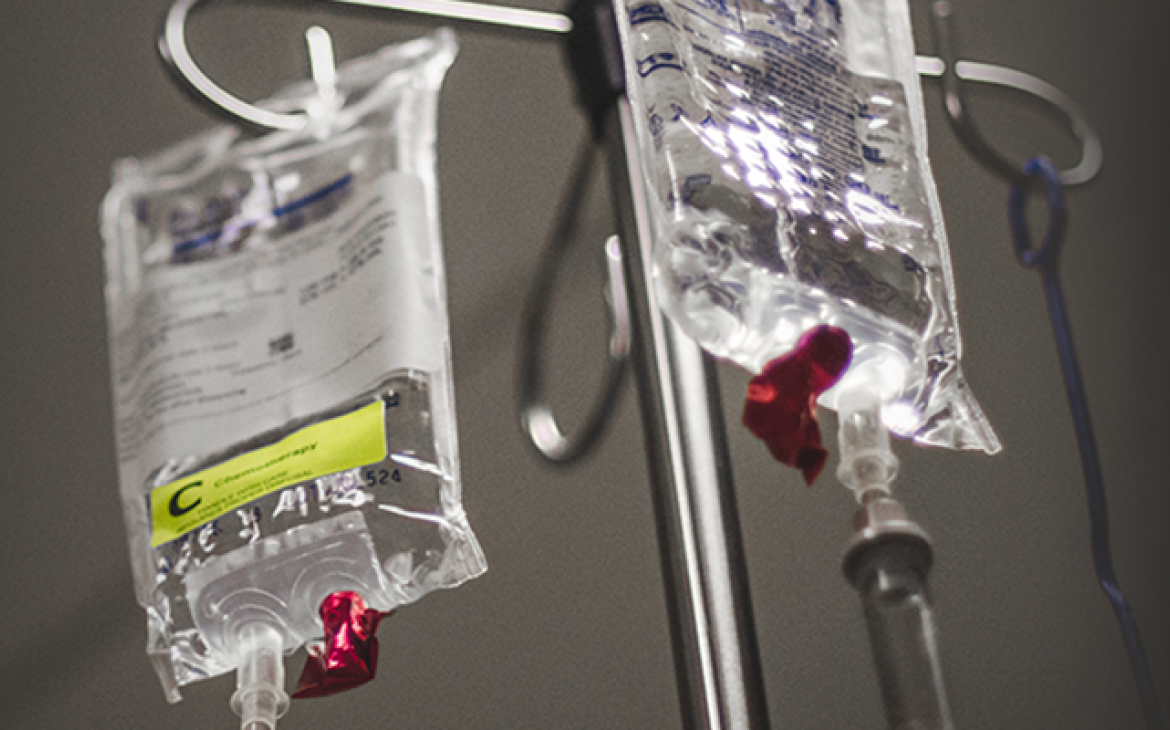
Quality assurance is a wide-ranging concept encompassing all factors that collectively influence the quality attributes of medical products. To support and strengthen quality assurance and related regulatory processes, regional and global collaboration is critical, panelists emphasized during an April 26 session of the Asia-Pacific Economic Cooperation (APEC) forum’s Medical Product Supply Chain Dialogue, co-hosted by the U.S. FDA and USP in Rockville, Maryland.
The panel was titled “Experiences Strengthening Quality Assurance in the APEC Region,” with participants hailing from the Center for Global Development; The Global Fund to Fight AIDS, Tuberculosis and Malaria (The Global Fund); the Food & Drug Administration of the Republic of the Philippines (FDA Philippines); and the Department of Health and Aged Care of Australia.
Collaboration builds trust and regulatory capability
Collaboration at a regional and global level takes time but “it creates and builds trust,” opined panelist Javier Guzman, director of global health policy and senior fellow at the Center for Global Development. Collaboration has been especially helpful in recent years in strengthening global medicines regulatory authorities, which play a key role in assuring the quality of medical products and guarding against the potential for substandard and falsified medicines.
“We should not underestimate the progress we’ve seen in quality assurance in the last decade,” Guzman said. For example, he touted development of the World Health Organization (WHO) Global Benchmarking Tool for evaluation of national regulatory programs for medicines as “the first…single integrated, agreed-upon framework to assess regulatory systems.” The tool provides a means to “move from immature [regulatory] systems to mature functional systems,” Guzman said. While WHO began assessing regulatory systems in 1997, work on the unified tool began in 2014 and it has subsequently incorporated various revisions in response to stakeholder feedback.
The WHO Prequalification (PQ) program also plays a critical role in ensuring that vital health products meet quality standards, including active pharmaceutical ingredients (APIs) and finished drug products. The program helps improve public health in low- and middle-income countries in particular.
FDA Philippines worked with the WHO PQ program during the COVID-19 pandemic, for example, to help make quality priority medical products available to those who urgently need them, explained panelist Jesusa Joyce N. Cirunay, director IV of the Center for Drug Regulation and Research, FDA Philippines. “We are not going to reinvent the wheel when a stringent regulatory authority has already made it available in the market and it’s freely sold,” Cirunay explained.
Based on progress to date, expanding the scope of drug products eligible for WHO prequalification and continued strengthening of global regulatory capability will further support improvements in quality assurance across the medicines supply chain.
Ensuring quality takes all stakeholders
As the panel discussion highlighted, all stakeholders have a role to play in quality assurance, including regulators, manufacturers, procurers, and distributors. However, coordination and collaboration between countries and among regional stakeholders is essential to regulatory strengthening initiatives in particular. USP collaborates with global regulators and other partners to strengthen regulatory systems around the world, including in low- and middle-income countries through its Promoting the Quality of Medicines Plus (PQM+) Program.
During the panel discussion, participants shared examples of how coordination and collaboration have facilitated their regulatory efforts. During the COVID-19 pandemic, “regulators were put under enormous pressure to make rapid decisions on the benefit to risk profile of vaccines manufactured using new technology with limited clinical data to allow vaccination programs to begin as quickly as possible,” recounted panelist Michael Wiseman, assistant secretary, International Regulatory Branch, Therapeutic Goods Administration, Department of Health and Aged Care, Australia. “Collecting real world safety data, including country-specific data, and information sharing was key to ensuring safety of COVID vaccines.”
The Global Fund operates in various regulatory environments and relies heavily on rigorous regulatory oversight. However, “we face a lack of knowledge on the quality assurance principles, and we have a lot of occasion to try to disseminate and educate,” noted panelist Alain Prat, team leader, quality assurance, Health Product Management Sourcing Department at The Global Fund. Referring to The Global Fund’s role in contributing to the quality of medications needed to fight AIDS, tuberculosis and malaria, Prat suggested some flexibility also can help during public health emergencies. “We have to improve and integrate [quality assurance] requirements with the principle of flexibility in order to face the next pandemic,” Prat said.
Standards strengthen quality assurance
USP works to support and strengthen quality assurance and related regulatory processes through a range of initiatives in the APEC region and beyond. This includes development of quality standards, guidelines and best practices; harmonization of standards across borders; providing technical assistance; and convening stakeholders to promote information sharing and discussion. Specific examples of USP resources that help ensure quality include those addressing substandard and falsified medicines and nitrosamine impurities. A separate panel during the APEC meeting addressed the topic of safeguarding patients from impurities in the drug supply chain.