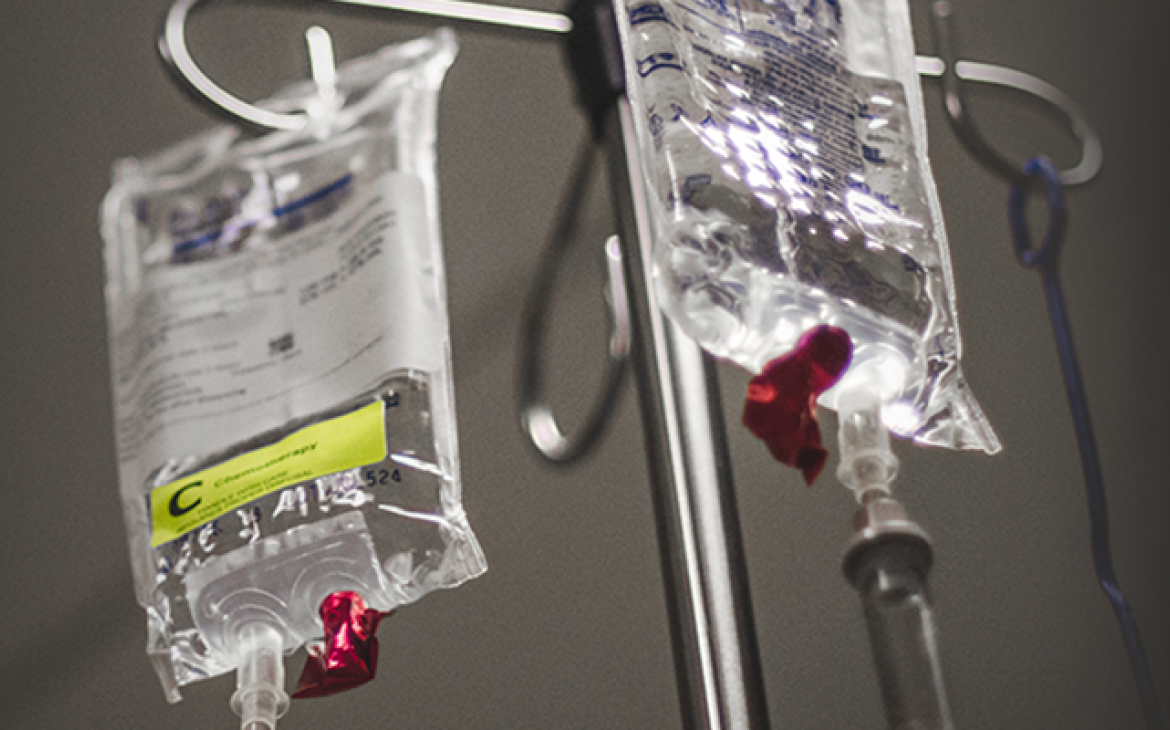
After Laura Bray’s daughter was diagnosed with cancer and began chemotherapy treatment, she faced three separate shortages of the life-saving drugs she needed, all within nine months. “All of them were different medicines, different causes,” recounted the founder and chief change maker at Angels for Change, a volunteer-supported organization on a mission to end drug shortages. Bray spoke during an April 25 panel session of the Asia-Pacific Economic Cooperation (APEC) forum’s Medical Product Supply Chain Dialogue, co-hosted by the U.S. FDA and USP in Rockville, Maryland.
Identification of upstream medicines supply chain risks can enable regulatory and industry action to reduce potential disruptions and shortages by informing risk mitigation strategies, public and private investment, as well as policy reforms that build more resilience, Bray and other panelists suggested. The panel was titled “Identifying Vulnerabilities in the Upstream Supply Chain.” Participants also included Stephen Maddocks, medicines supply resilience lead, Medicines Supply Branch, Medicines Directorate, Department of Health and Social Care, United Kingdom; and Tony Sardella, senior research advisor, Center for Analytics and Business Insights, Washington University in St. Louis.
The panel highlighted three key factors that can increase a medication's risk for shortage: low prices, geographic concentration of sourcing, and quality concerns. Those factors are also frequently interrelated. During the discussion, Bray emphasized the connection between quality and economic factors, Maddocks highlighted the pressure of economic factors on supply, and Sardella stressed how low margins for some drugs can affect a manufacturer’s ability to reinvest profits in quality advances, manufacturing innovation, and manufacturing redundancies.
Lower-priced drugs vulnerable to shortages
Lower-priced drugs – which include generics with lower profit margins for manufacturers – are known to have a higher risk of shortages since they offer limited incentives for manufacturers to stay in or enter the market. In fact, a “lack of incentives for manufacturers to produce less profitable drugs” was cited as root cause number one in FDA’s 2019 report Drug Shortages: Root Causes and Potential Solutions. The “lack of a measurable product differentiation is a critical contributor to price erosion in [the generic drug] industry,” Sardella noted. “The generic industry is built to have no differentiation. Exact same medicine, similar equivalence.” To improve margins, some industry participants have sought to reduce manufacturing costs by concentrating production in lower-cost geographies, Sardella observed. However, this concentration of sourcing can increase supply chain vulnerabilities.
Geographic concentration and drug shortages
Drugs with greater geographic concentration in manufacturing of their active pharmaceutical ingredient (API) and/or finished dose form are known to be more susceptible to possible shortages due in part to the potential concentrated impact of external events like natural disasters (e.g., earthquakes, hurricanes), trade wars, domestic or geopolitical strife, or pandemics such as COVID-19. Geographic diversification of sourcing is needed to bolster medicines supply chain resilience, though Maddocks suggested it’s not just about having two or three different manufacturing sites, but having them in different geographies to help spread the risk.
Quality concerns contribute to risk
Pre-pandemic, quality problems were responsible for the vast majority of drug shortages – at over 60% – according to FDA’s 2019 analysis. While an increasing number of demand-related shortages are occurring now, the panel discussion underscored that quality and medicines supply chain resilience are inextricably linked. While issues with medicines quality can threaten supply chain resilience, supply chain disruptions can also lead to quality issues. For example, increased proliferation of substandard and falsified medicines can stem from drug shortages through high demand for scarce supplies and economic incentives for fake medicines to enter the market. Meanwhile, an observed decline in the rate of FDA warning letter close-outs could be an indicator of the inability of the generic drug industry to reinvest in advances in quality and manufacturing innovation, Sardella speculated.
Identifying vulnerabilities as part of the solution
Panelists concluded that the supply chain would be more resilient and reliable if solutions are targeted at drugs found to be at particular risk of shortage. Channeling investments and policy reforms needed to ensure resilience depends in part on access to data and insights that allow understanding of potential supply chain vulnerabilities.
USP’s work in this area includes development of an early-warning capability for potential disruptions in the upstream medicines supply chain. Known as the USP Medicine Supply Map and launched in 2021, this capability leverages more than 250 million data points spanning 92% of generic medicines approved in the U.S. in a platform that assesses the vulnerability of specific medicines to supply chain disruptions.