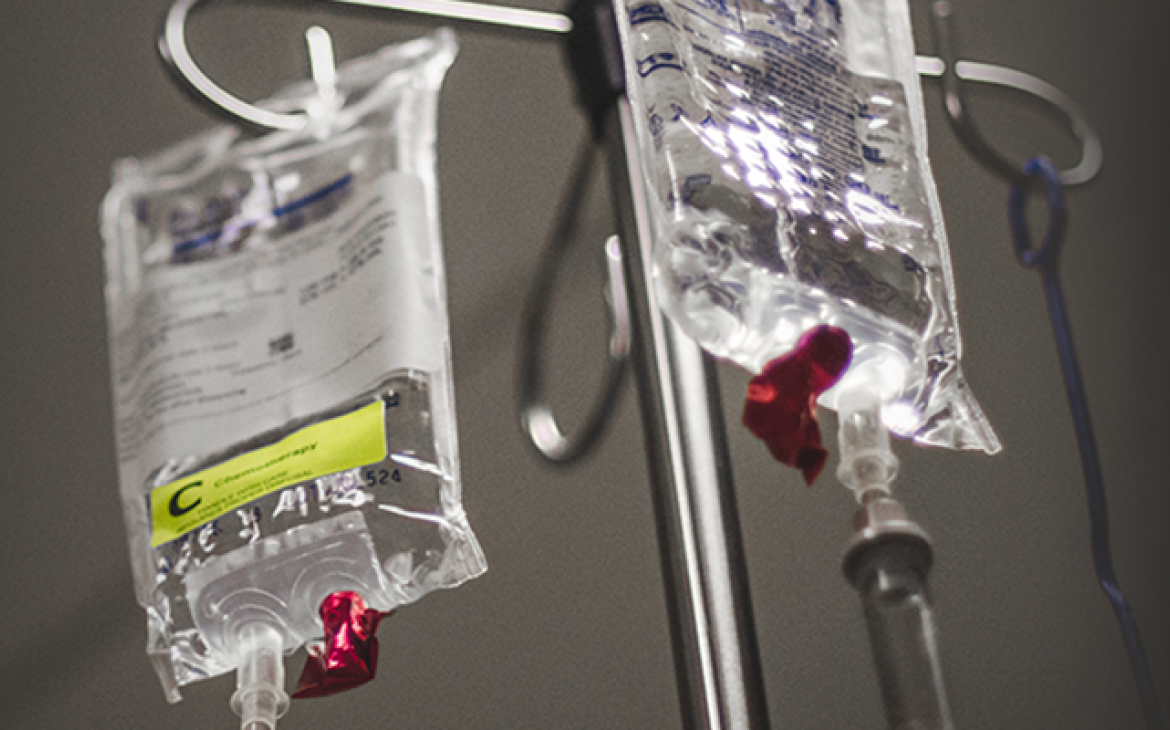
For the first time in more than 20 years, U.S. regulators are considering the reintroduction of bovine (cow-derived) heparin into the U.S. An essential and commonly-used drug, heparin helps to prevent blood clots from forming in patients undergoing heart surgeries, blood transfusions and dialysis.
Today, all heparin products in the U.S. are derived from pigs. Seventy-five percent of the crude porcine heparin used to make active pharmaceutical ingredients (API) comes from outside of the U.S., with a majority of that percentage originating from China. The reintroduction of bovine heparin into the U.S. market would expand sources for this important drug, thus helping to address concerns about potential shortages and product adulteration.
Concerns about bovine sources
Prior to the early 1990s, bovine heparin was widely available and used in the U.S. The first bovine heparin in this country was approved in 1939, with several other heparins entering the market after that initial approval. The products were found to be safe and effective, and no adverse events associated with their use were ever reported.
In the late 1980s, however, cases of bovine spongiform encephalopathy (BSE) -- also known as “mad cow disease” -- in the United Kingdom generated concerns about the use of heparin from bovine sources. This eventually led to the voluntary withdrawal by manufacturers of all bovine heparin products from the U.S. market. Since that time, all heparin products approved in the U.S. and Europe have been solely sourced from pigs.
Adulterated heparin
Heparin became global headline news from 2007-2008 when adulterated heparin was suspected of being connected to nearly 250 deaths and over a hundred adverse reactions reported to the U.S. Food and Drug Administration (FDA). Investigations eventually linked the cases of adulteration to crude heparin sourced from China.
In 2007, a viral infection known as blue-ear disease swept through China, wiping out pig populations at an alarming rate. As the blight drove up the price of crude porcine heparin, it was concluded that over-sulfated chondroitin sulfate (OSCS) was substituted for some of the actual heparin. OSCS costs far less, and was able to “fool” existing quality tests.
The heparin crisis opened the eyes of the American public to the threat of economically-motivated adulteration of medicines and the potential vulnerability of domestic drug supplies in increasingly global manufacturing supply chains. It also identified underlying concerns associated with reliance on one country as a primary source for the supply of a critical drug like heparin.
Reintroducing bovine heparin into the U.S.
Last year, the FDA hosted a meeting with its Science Board to discuss the possible reintroduction of bovine heparin in the U.S. With today’s limited sources for the global supply of porcine heparin and little growth potential for these products to be manufactured in other parts of the world such as U.S. and Europe, the FDA is concerned about the emergence of potential shortage situations. Also, the experience of 2007-2008 underscored the risk of heavy reliance on single-animal and single-country sourcing when factors like blue-ear disease can have such a dramatic impact on one medicine’s supply.
This August, the U.S. Pharmacopeial Convention (USP) will host its “6th Workshop on the Characterization of Heparin Products” in Brazil. A major focus of the meeting will be on bovine heparin, many suppliers and manufacturers of which are located in Latin America. In spite of concerns about mad cow disease, bovine heparin was never removed from the Brazilian market and the risks associated with BSE are now better understood than they were 20 years ago.
The goals of the workshop will be to generate a better understanding of the differences between porcine and bovine heparins, the clinical implications of reintroducing bovine heparin and the broader ramifications of bovine heparin in the U.S. market. Given the significant changes that have occurred in manufacturing practices over the last 20 years, USP is also gathering data on bovine heparins that have been marketed in other parts of the world in order to gain an improved understanding of differences between porcine and bovine when it comes to product quality.
To learn more about USP’s standards for heparin and other biologics, go to: http://www.usp.org/usp-manufacturers/biologics-biotechnology.
Anita Szajek, Ph.D., is a principal scientific liaison in USP’s Department of Biologics & Biotechnology.